Count down to safe patient handling
The deadline for compliance with the final phase of New York State’s Safe Patient Handling (SPH) Act is fast approaching. The Act became law in 2014 as a result of advocacy by NYSNA and our union allies and patient advocacy groups. Come January 1, individual healthcare facilities will be required to move beyond the establishment of SPH planning committees and put SPH programs into place.
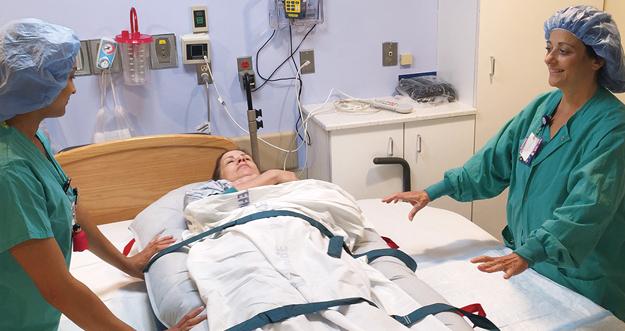
Safe patient handling is defined under the Act as a practice that creates a safe environment for patients and healthcare workers by eliminating hazardous manual lifting tasks through technologies such as mechanical lifts. Healthcare workers have one of the highest occupational injury rates, particularly back and other musculoskeletal injuries, leading to a considerable amount of lost work time.
New York hospitals and other accredited medical facilities are at various stages of compliance with the upcoming deadline. Two NYSNA hospitals are profiled here: Staten Island University Hospital (SIUH), a large (714-bed) facility that is part of the Northwell Health System; and Flushing Hospital Medical Center, a smaller (293-bed) community hospital located in Queens.
SIUH
NYSNA RN Kelly Moed pioneered an SPH program at Staten Island University Hospital in 2007 which has become a national model. She served as a member of the NYS Health Commissioner’s statewide SPH workgroup during the first phase of the Act’s implementation. In that role, she reviewed existing SPH programs in New York and beyond, identified sample SPH policies and best practices, and helped compile training materials for statewide use.
She attributes the success of SIUH’s program to the fact that frontline caregivers are fully integrated into the program. “SIUH’s administrators take workplace safety very seriously and have a very clear understanding of the tremendous return on SPH investment,” said Ms. Moed.
With SIUH so far ahead of the regulatory deadline, it has been able to collect years of data and analyze the program’s impact. Ms. Moed said, “Every single month the SPH committee reviews injuries, tallies lost and modified work days, tracks trends and makes recommendations for necessary changes. Each manager is responsible for reporting the results of her or his investigation of each staff injury resulting from patient handling. The committee decides if the injury was preventable and makes recommendations for how things could be done better.”
Within three years of implementation, SIUH reduced lost and modified work time by more than 60% through a combination of injury prevention and a return-to-work program that pools jobs available for those unable to return to full duty. “It’s win-win because it enables staff who are able and willing to keep working — but in jobs that don’t compromise their health.”
SIUH is now at the point where most staff understands the value of SPH for workers as well as patients. “After air assisted transfer devices were introduced in Labor and Delivery, caregiver injury rates fell and patient satisfaction increased. And L&D became one of SPH’s biggest champions.”
“There is no question that the equipment purchases have paid for themselves many times over through the drop in lost work time, better patient outcomes, and higher patient satisfaction — which ultimately lead to higher reimbursement,” said Ms. Moed.
Her experience has taught her that work on SPH doesn’t end after the hospital makes its first equipment purchase. “Success requires ongoing interdisciplinary committee work to measure the return on investment and to keep abreast of necessary changes,” she said. “It’s a feedback loop that builds on each new experience.”
Flushing Hospital
Flushing Hospital RN and NYSNA Director at Large Tracey Kavanagh is proud of her hospital: “For a community hospital, Flushing has taken a leadership role in complying with the SPH law.”
In October 2015, the hospital sent Ms. Kavanagh and Michelle Jones, RN, to a Safe Patient Handling workshop at the Greater New York Hospital Association to learn about how to get the SPH process rolling inside their hospital.
Soon after, Flushing established its SPH Committee. NYSNA RNs Johanna Pinzon and John Hartin have spent the past several months working with nurses’ aides, managers and other frontline caregivers on a unit-by-unit assessment.
“We’ve learned that there is no ‘one-size fits all’ solution. Every unit has unique needs, and those needs change,” said Ms. Pinzon. “In cardiac, we were accustomed to dealing with patients up to 200 pounds. Once we added bariatric services we needed the appropriate equipment for patients who weigh twice that amount.”
The committee is now assessing equipment and arranging for on-site trials. “We’ve learned that what works in other hospitals may not work at Flushing. Size constraints unrelated to budget will limit the equipment we can pursue. It’s like buying a couch for your apartment: you have to make sure it will fit through the door.”